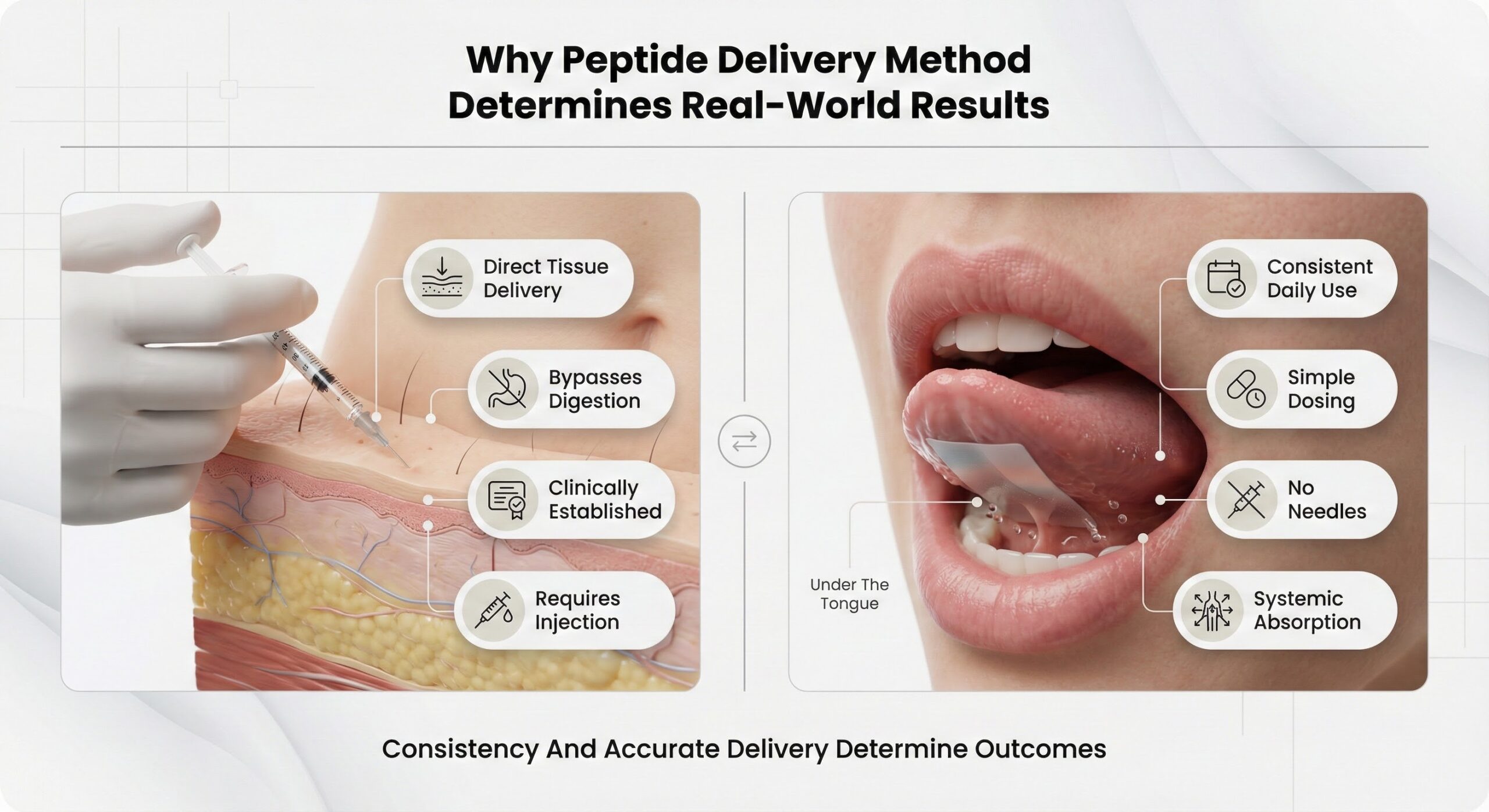
Why Peptide Delivery Method Determines Real-World Results
Peptides regulate cellular repair, metabolic function, immune response, and body composition through precise receptor signaling. People using peptides report improvements in recovery time, energy regulation, tissue healing, and physical performance. These benefits depend entirely on one factor: delivering the peptide into your bloodstream at the correct dose, consistently, every single day.
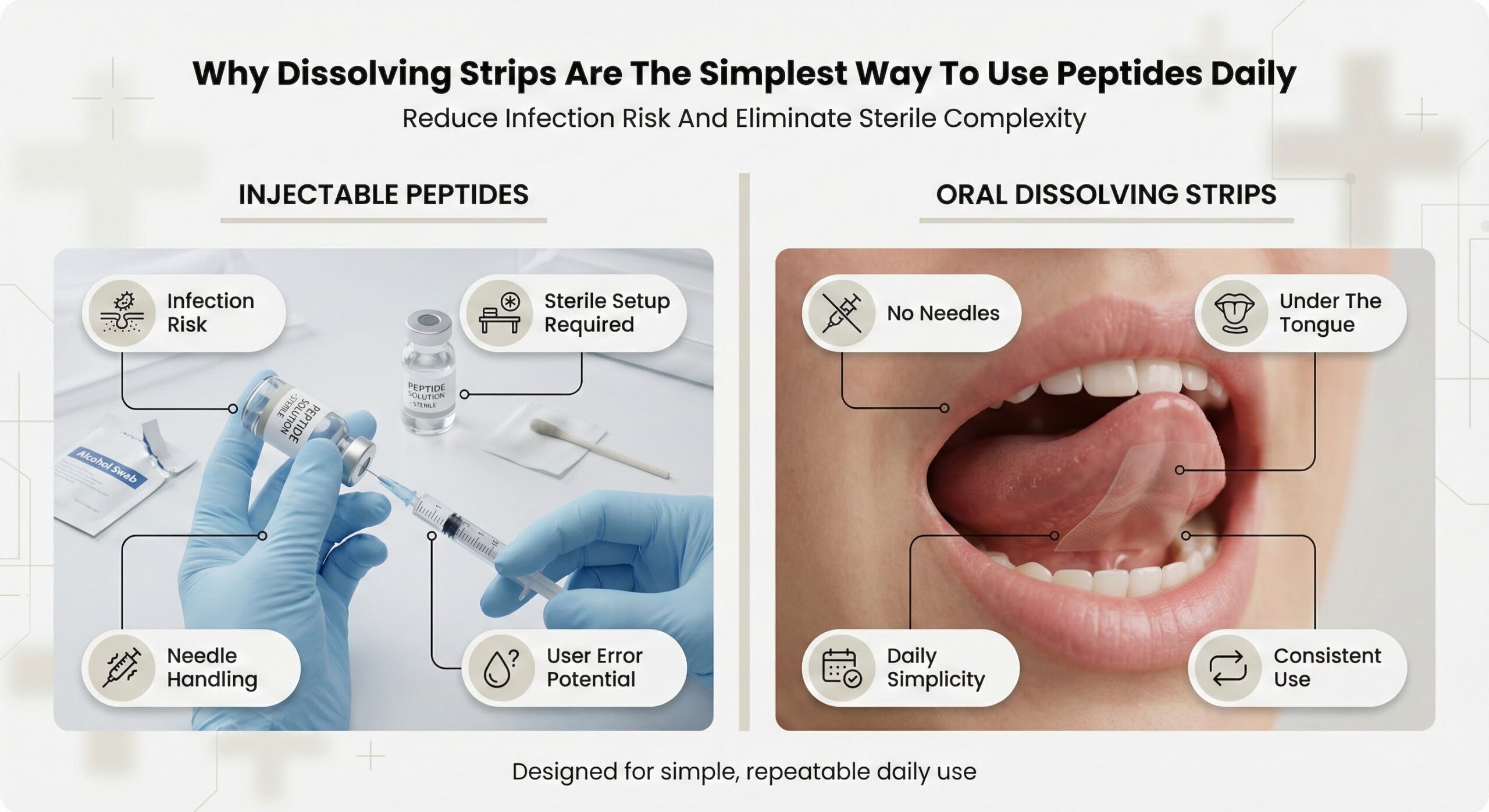
The delivery method you choose determines whether that happens. Subcutaneous injections have been the clinical standard for decades because they bypass digestive breakdown and deliver peptides directly into tissue. Oral dissolving films—thin polymer strips that release peptides through the tissue under your tongue—offer a simpler system that eliminates the multi-step process injections require. Both methods work. The question is which one supports daily adherence without introducing variables that compromise dosing accuracy.

What Peptides Do in the Body
Peptides are short chains of amino acids that function as signaling molecules. They bind to specific cellular receptors and trigger biological processes including tissue repair, hormone regulation, immune modulation, and metabolic control. Because they mimic natural signaling pathways, peptides offer therapeutic effects with precision that synthetic drugs often cannot match.
Their effectiveness, however, requires consistent delivery. Missing doses, delivering inconsistent amounts, or allowing degradation before the peptide enters circulation eliminates the benefits entirely.[1]
How Subcutaneous Injections Work
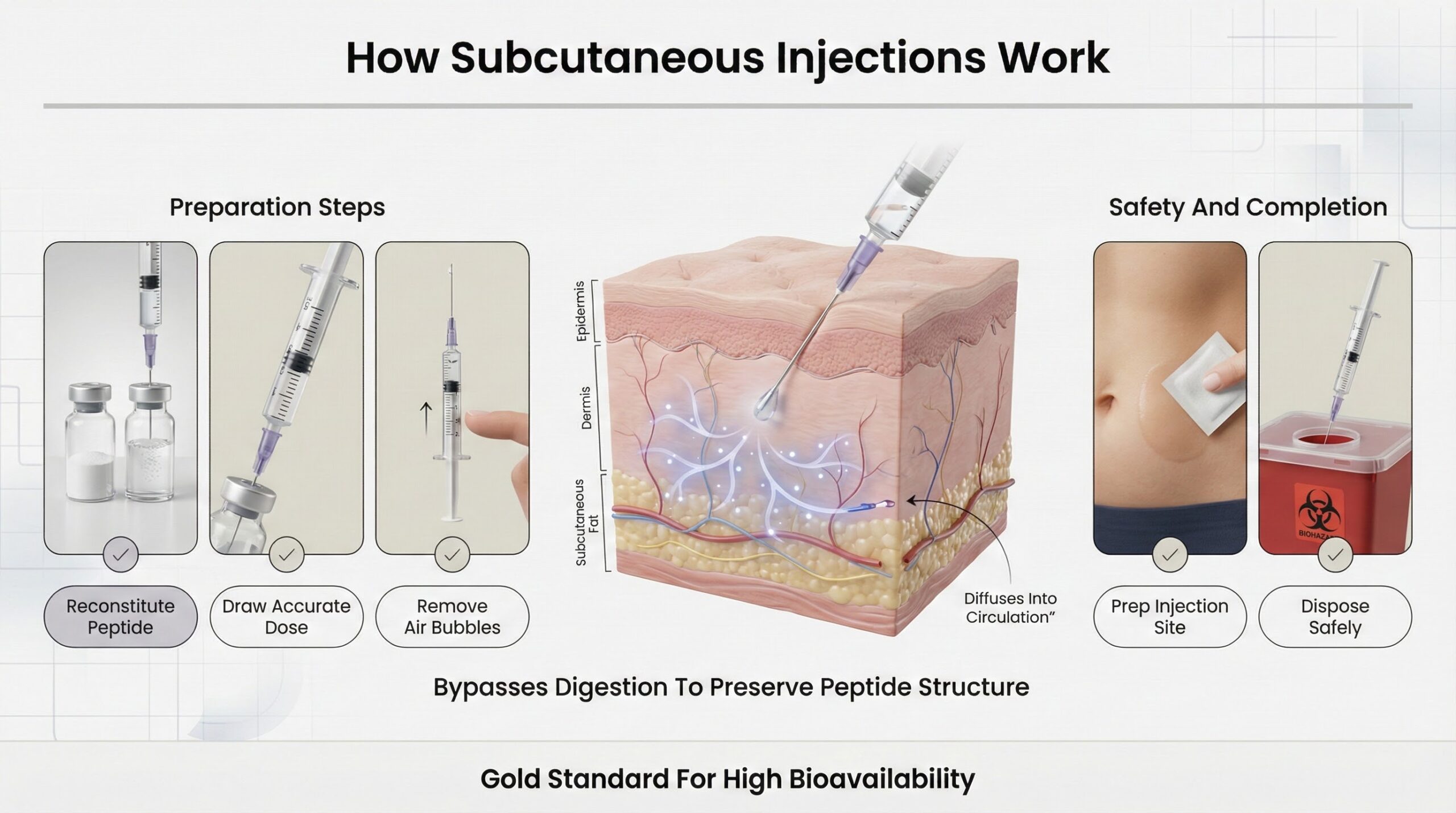
Subcutaneous injections place a liquid peptide formulation into the fatty tissue beneath the skin, where it diffuses into nearby capillaries and enters systemic circulation. This method has been the gold standard because it avoids the digestive system entirely, preserving peptide structure and delivering it with high bioavailability.
The process involves reconstituting lyophilized peptide powder with bacteriostatic water, drawing the dose into a syringe, checking for air bubbles, swabbing the injection site, and disposing of sharps safely. Each step must be executed correctly for the therapy to work as intended.

Where the Injection System Breaks Down
Research on insulin administration using syringes and vials found that healthcare professionals—trained, experienced nurses—made significant dosing errors even under controlled conditions. For a 2-unit insulin dose, the median absolute percentage error was 30%. In the worst cases, errors exceeded 2 units, meaning more than double the intended dose was administered.[2]
The most common failure was skipping the air bubble check, which occurred in 42% of trials. Other factors included pressure differentials in the vial, difficulty measuring micro-doses, and inconsistent vertical insertion during the draw phase. These aren't user failures—they're system-level friction points inherent to multi-step injection protocols.[2]
Once reconstituted, peptides in liquid form face immediate stability challenges. They degrade through hydrolysis, aggregation, and precipitation—processes that accelerate with exposure to air, temperature fluctuation, and time. Peptides stored in aqueous solution require refrigeration and have shelf lives measured in weeks. Even under ideal conditions, potency decreases as chemical degradation progresses.
Subcutaneous injections also carry infection risk when sterile technique lapses. Failing to clean the skin, using contaminated needles, or skipping hand-washing increases the likelihood of bacterial infections at the injection site. Repeated injections in the same area can cause tissue hardening and localized inflammation.
How Oral Dissolving Films Work
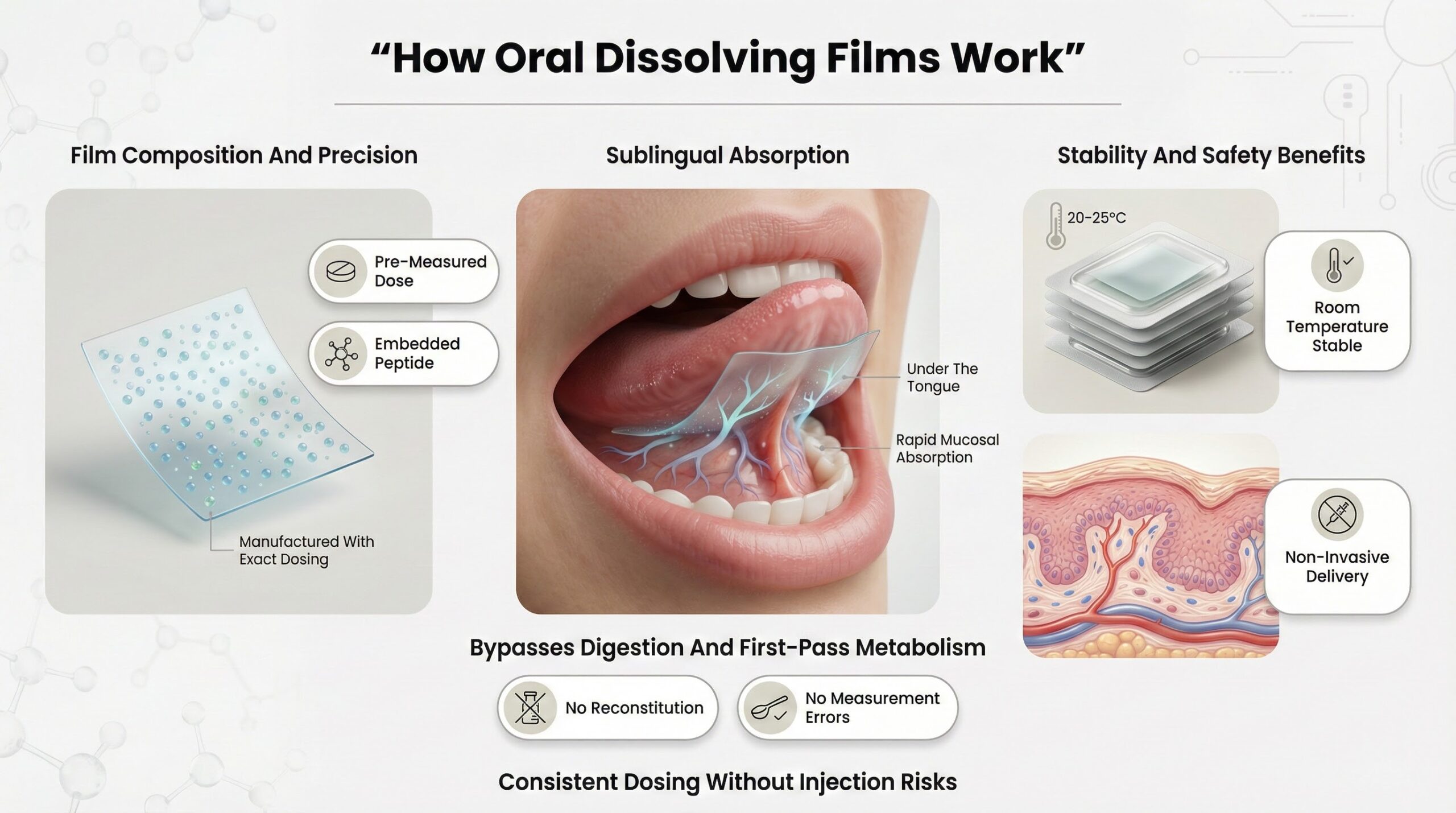
Oral dissolving films are thin polymer sheets embedded with the active peptide. When placed under the tongue, the film disintegrates in seconds and releases the peptide for absorption through the oral mucosa. This route bypasses the stomach's acidic environment and first-pass liver metabolism, both of which would degrade swallowed peptides.
The key advantage is elimination of user-dependent dosing variables. The peptide dose is manufactured into the film with precision during production, meaning every strip contains the exact amount intended. There is no reconstitution, no measurement, no air bubbles, and no sterile technique required.[3]
Because the peptide is embedded in a dry polymer matrix, it remains protected from hydrolysis and aggregation. The solid-state formulation eliminates the degradation issues seen in liquid peptide vials. Oral films can be stored at room temperature without significant potency loss, extending shelf life and removing refrigeration requirements.
Oral films are non-invasive. There is no needle, no puncture wound, and no opportunity for bacterial contamination at an injection site. The primary risk is mild oral mucosal irritation, which resolves quickly.
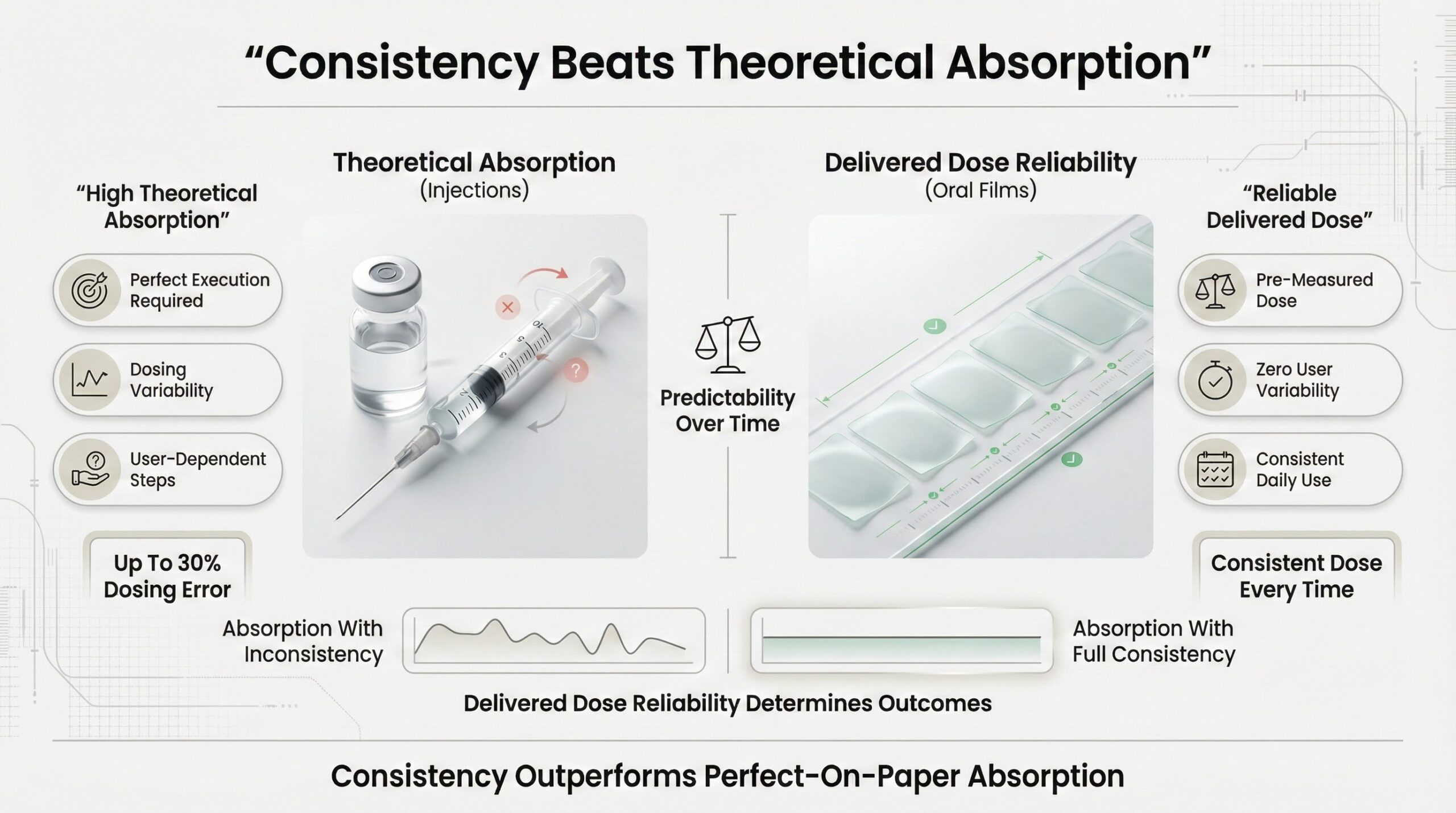
Consistency Beats Theoretical Absorption
Sublingual bioavailability for peptides varies depending on formulation. Without permeation enhancers, absorption through the oral mucosa can be limited. Modern formulations use mucoadhesive polymers and absorption enhancers to improve uptake, achieving bioavailability rates that support meaningful clinical outcomes.[4]
Injections offer higher theoretical absorption when executed perfectly. But dosing errors of 30% or more are common even among trained users. A delivery system with 90% bioavailability but 30% dosing inconsistency delivers less predictable outcomes than a system with 35% bioavailability and zero dosing error.
The real comparison is not absorption percentages—it's delivered dose reliability over time.[5]
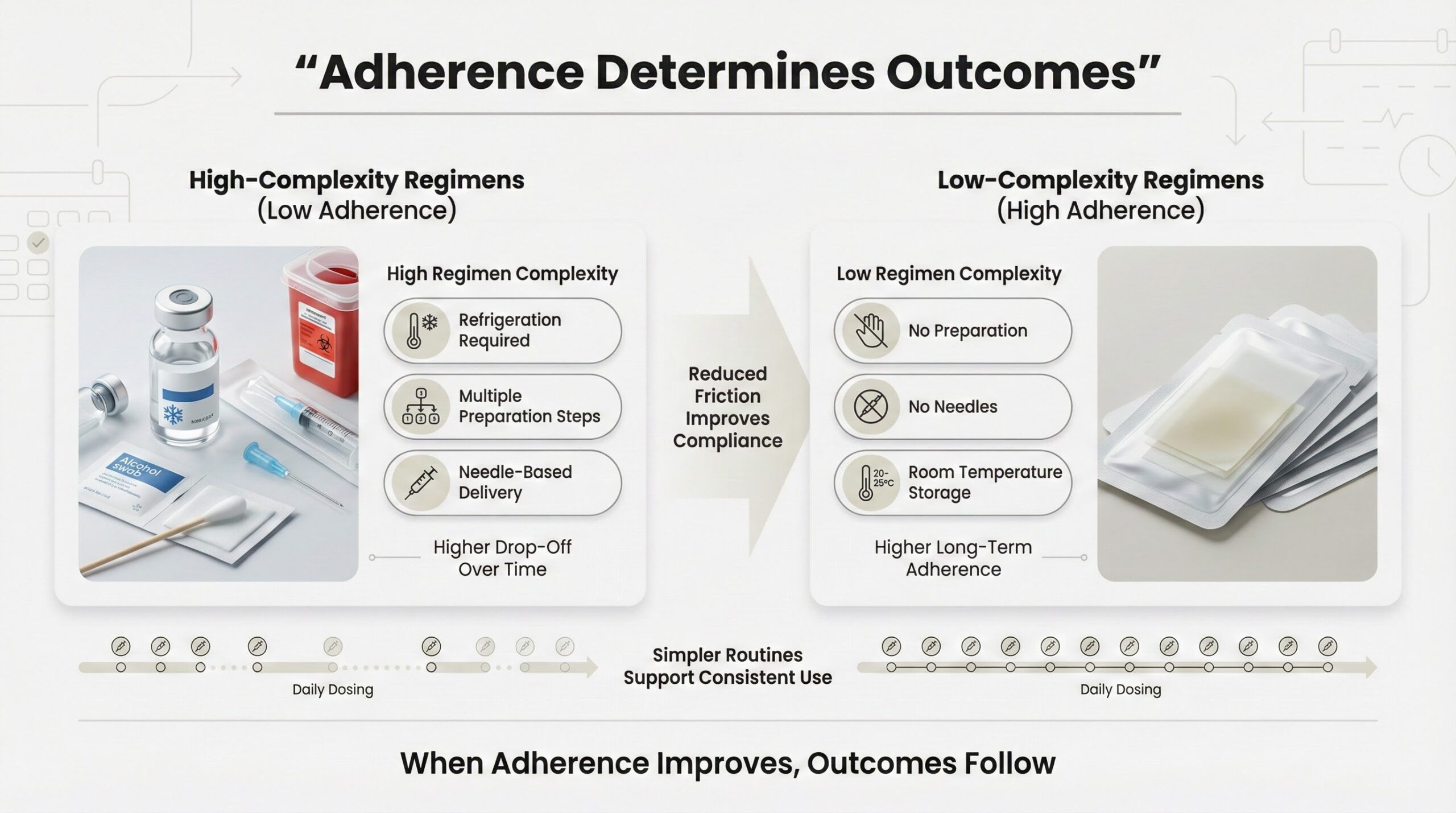
Adherence Determines Outcomes
Medication adherence research consistently shows that regimen complexity is the primary barrier to long-term compliance. Therapies requiring refrigeration, preparation steps, and needle-based administration have lower adherence rates than simpler alternatives. Studies on long-term medication use found that patients with low-complexity regimens were significantly more likely to remain adherent than those with high-complexity protocols.[1]
Oral films address the behavioral dimension of peptide therapy directly. They dissolve in seconds, require no preparation, and do not trigger needle phobia—a documented barrier to injectable therapy adherence. By removing friction from the daily routine, adherence improves, and outcomes follow.
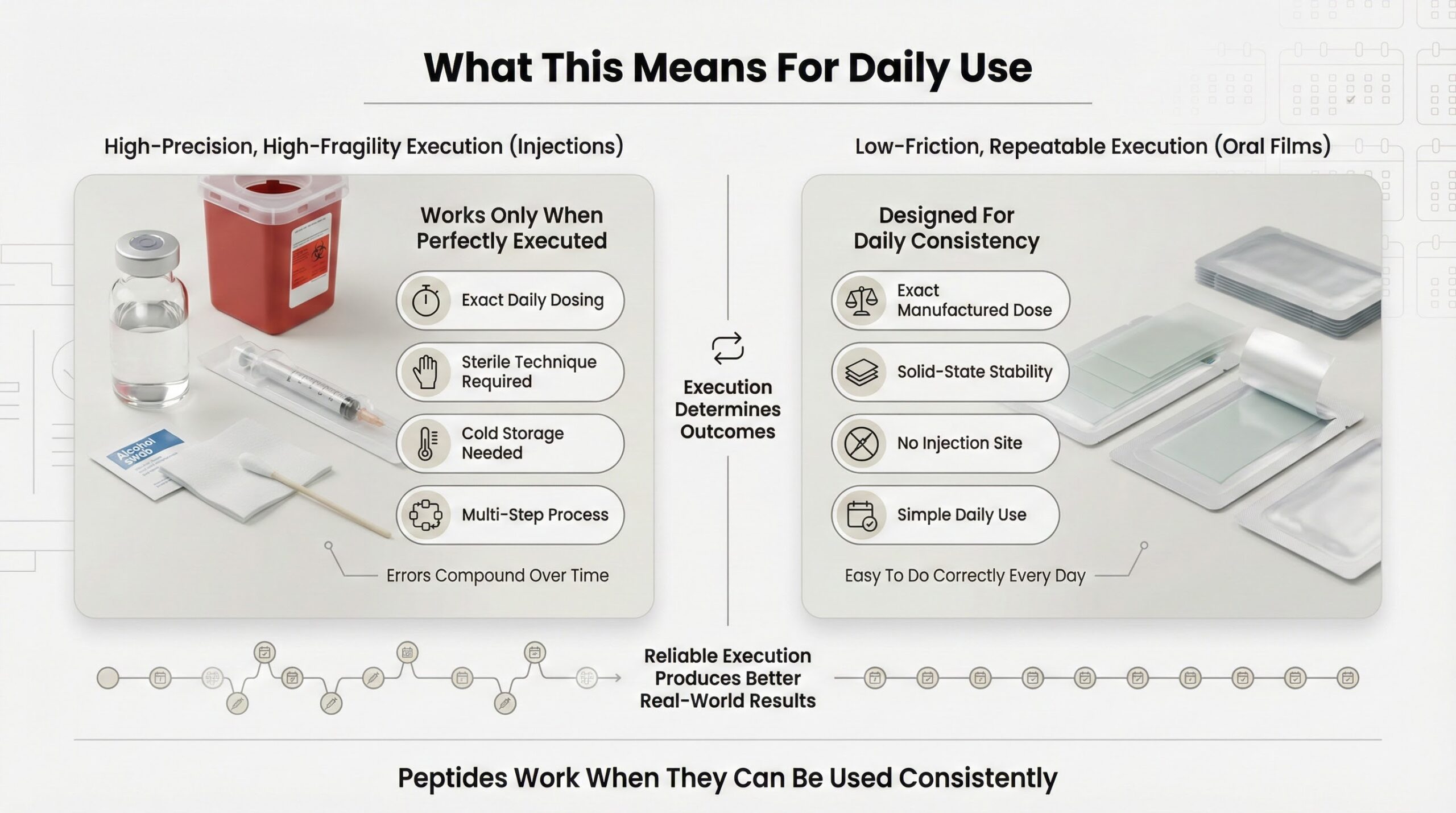
What This Means for Daily Use
Peptides deliver meaningful benefits for tissue repair, metabolic regulation, immune function, and recovery when used consistently. Subcutaneous injections work when performed correctly every day, at the exact dose, with proper sanitation and storage. But that execution depends on completing a multi-step process without error—something that fails frequently even under ideal conditions.
Oral dissolving films eliminate those failure points. The dose is exact because it is manufactured into the film. The peptide is stable because it is in solid form. There is no injection site, so there is no infection risk. The therapy works because it is simpler to execute correctly, every single day.[3]
For daily peptide use, the method that supports reliable, repeatable execution produces better real-world outcomes than the method with higher theoretical bioavailability but lower practical adherence. Peptides work. Oral dissolving strips let you work with them consistently.[5]
References
- Alhewiti A "Adherence to Long-Term Therapies and Beliefs about Medications." Int J Family Med. 2014. [View Study]
- Kondo M et al. "Analysis of factors affecting the accuracy of low-dose insulin dosage using syringes and vials: a cross-sectional study in a Japanese regional hospital." Diabetol Int. 2024. [View Study]
- Palezi SC et al. "Oral disintegration films: applications and production methods." J Food Sci Technol. 2023. [View Study]
- Renukuntla J et al. "Approaches for enhancing oral bioavailability of peptides and proteins." Int J Pharm. 2013. [View Study]
- [View Study]
- Zhang Z et al. "Discovery of peptides as key regulators of metabolic and cardiovascular crosstalk." Cell Rep. 2025. [View Study]
- Perrottet N et al. "Biases affecting injected doses of an experimental drug during clinical trials." Trials. 2016. [View Study]
Read More

What GMP Certification Means for Supplement Quality
March 10, 2026
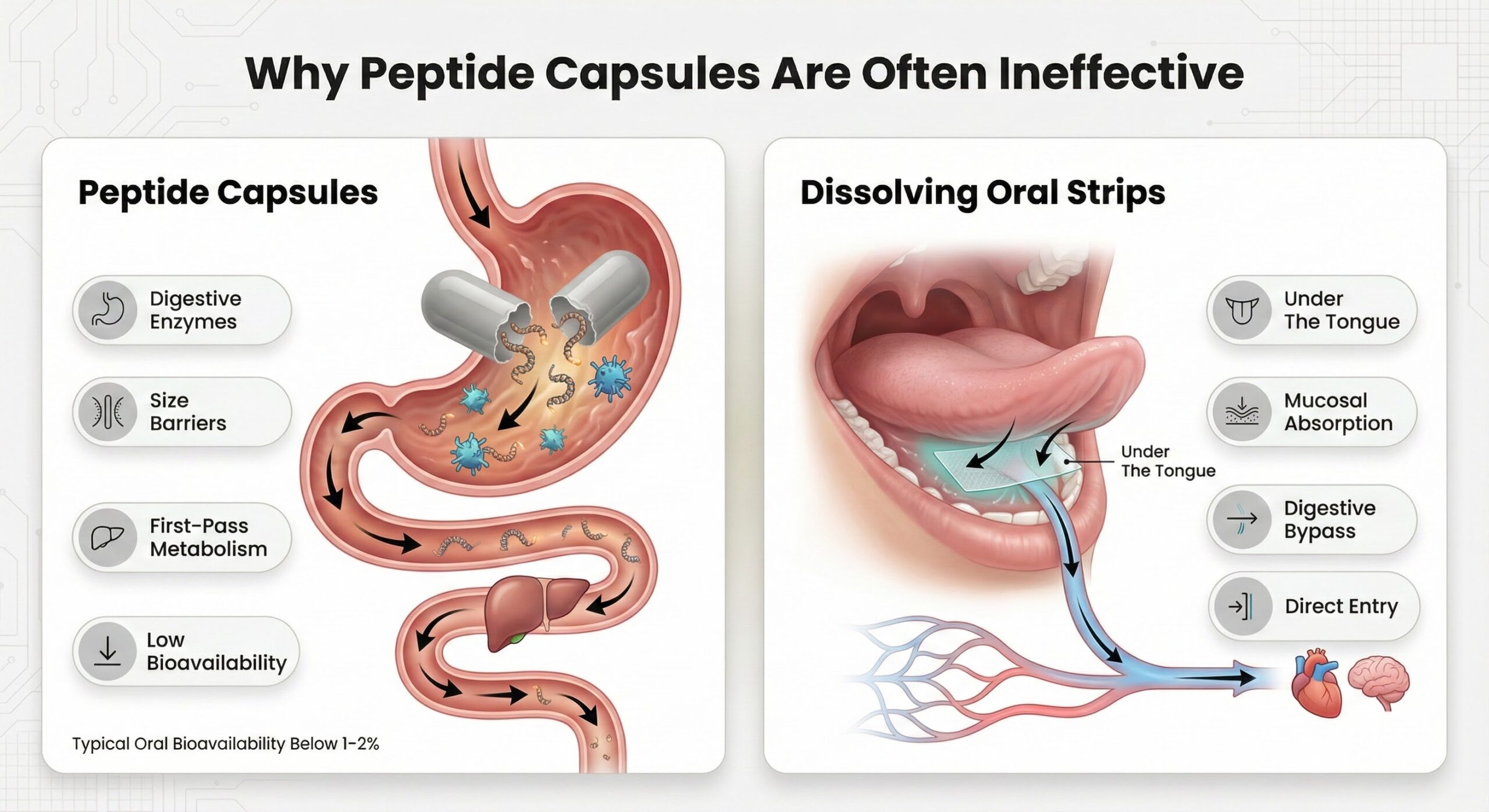
Why Peptide Capsules are Often Ineffective
March 10, 2026