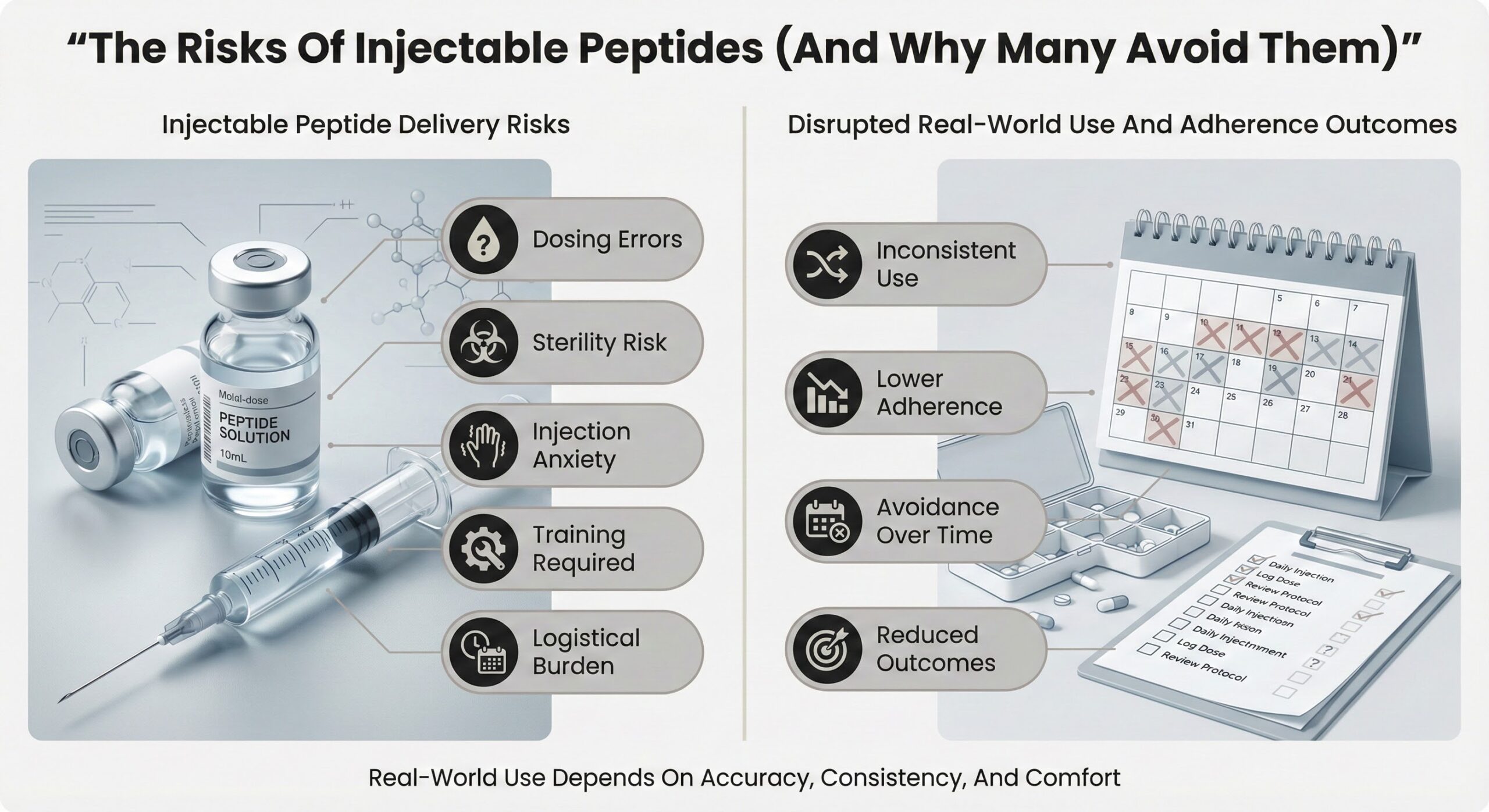
The Risks of Injectable Peptides (And Why Many Avoid Them)
Peptides can reliably support tissue repair, metabolic health, and recovery when they are delivered in a way that people can use accurately and consistently over long periods of time. Injectable systems often break that link between potential and real‑world outcome by layering in technical, logistical, and psychological failure points that many users understandably avoid.[1]

Why injection became the norm
Peptides are fragile chains of amino acids that are rapidly broken down by enzymes and acidic conditions in the digestive tract, leaving typical oral bioavailability at or below about 1–2% for most molecules. To bypass that loss, most peptide drugs have historically been delivered by subcutaneous or intramuscular injection, which lets them reach the bloodstream intact and sidestep first‑pass metabolism in the liver.
This shift to injection solves the stability problem but creates a demanding delivery system that depends on user skill. Over time, the complexity of that system is what tends to determine whether a peptide works in practice, not just its pharmacology on paper.
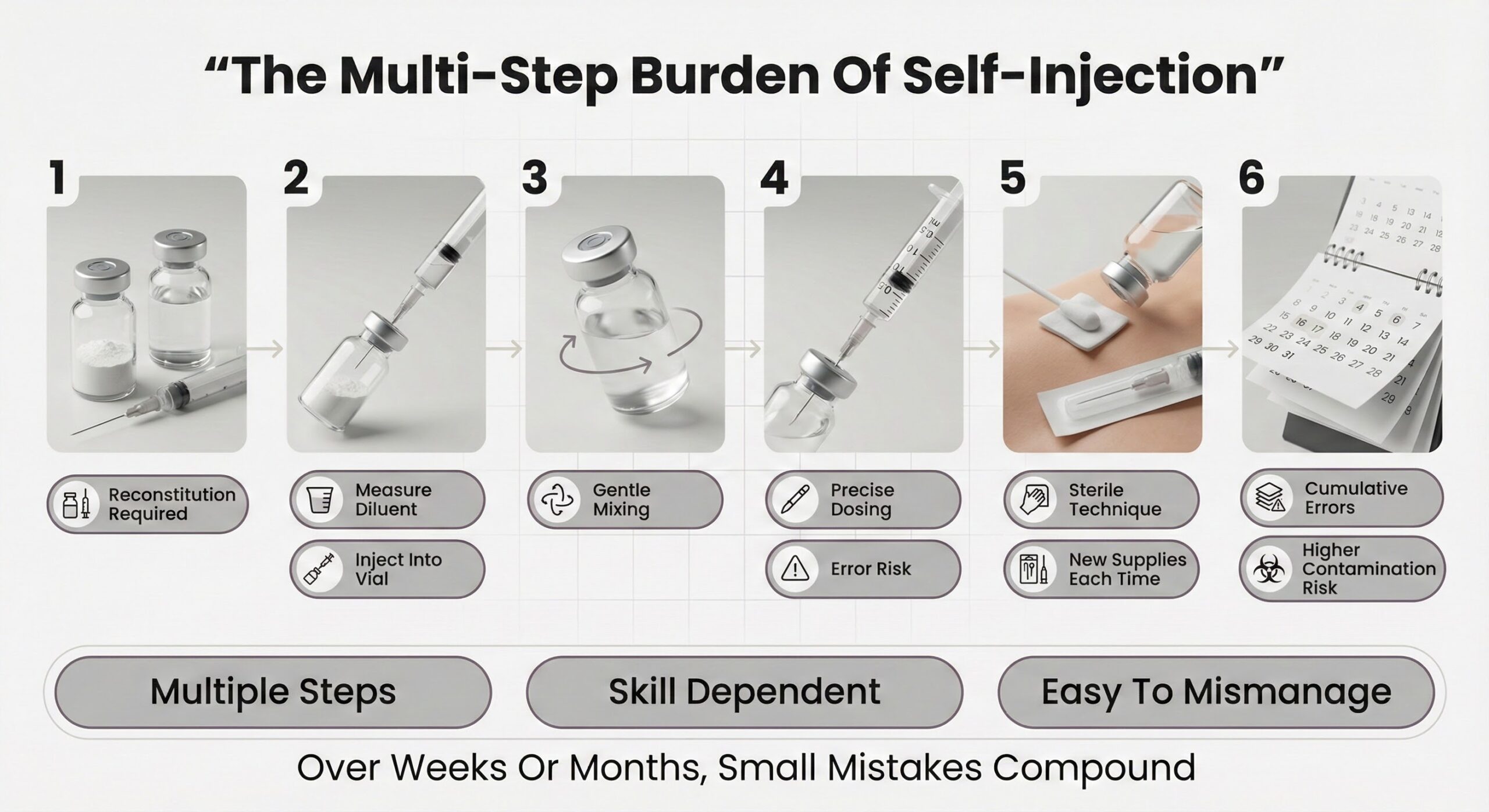
The multi‑step burden of self‑injection
Self‑injectable peptides typically arrive as a dry (lyophilized) powder that must be reconstituted with sterile diluent before use, which means the user is effectively doing miniature compounding at home. Every step—drawing up bacteriostatic water, injecting it into the vial, gently mixing, and withdrawing precise doses—creates room for under‑ or overdosing and for mishandling that can damage the peptide structure.[2]
Maintaining sterile technique is another constant demand: users must clean vial stoppers and skin, use new needles and syringes, and avoid touching critical surfaces to limit bacterial contamination and local infection. These tasks are straightforward for a nurse doing a few injections per day, but for an individual doing this at home for weeks or months, the cumulative chance of small errors—and therefore suboptimal results—increases.

Storage, reactions, and needle resistance
Reconstituted peptide solutions are generally less stable than their powder form and often require refrigeration with protection from heat and light to maintain activity. For anyone traveling, commuting, or juggling work and family routines, keeping a cold chain intact and timing doses around access to a refrigerator adds friction that directly affects whether doses are taken as intended.
On top of this, injectable peptides can cause local reactions such as redness, swelling, itching, or small raised areas at the injection site, especially early in use. While usually mild, more severe redness, pain, or systemic symptoms signal potential infection and understandably make users more hesitant to continue frequent injections. Repeated injections in the same area can also change the underlying fat tissue, which is why site rotation is recommended—another procedural detail that has to be done correctly to protect both comfort and absorption.
Psychologically, a large proportion of adults report needle fear or phobia, with surveys showing meaningful needle fear in up to one‑fifth or more of the population, and some studies finding much higher levels of needle discomfort or avoidance. In chronic therapies like growth hormone replacement, switching from daily to weekly injections has been shown to improve adherence, patient preference, and satisfaction while maintaining similar efficacy, underscoring how reducing injection frequency alone can lower drop‑off and adverse‑event rates over time.[3]
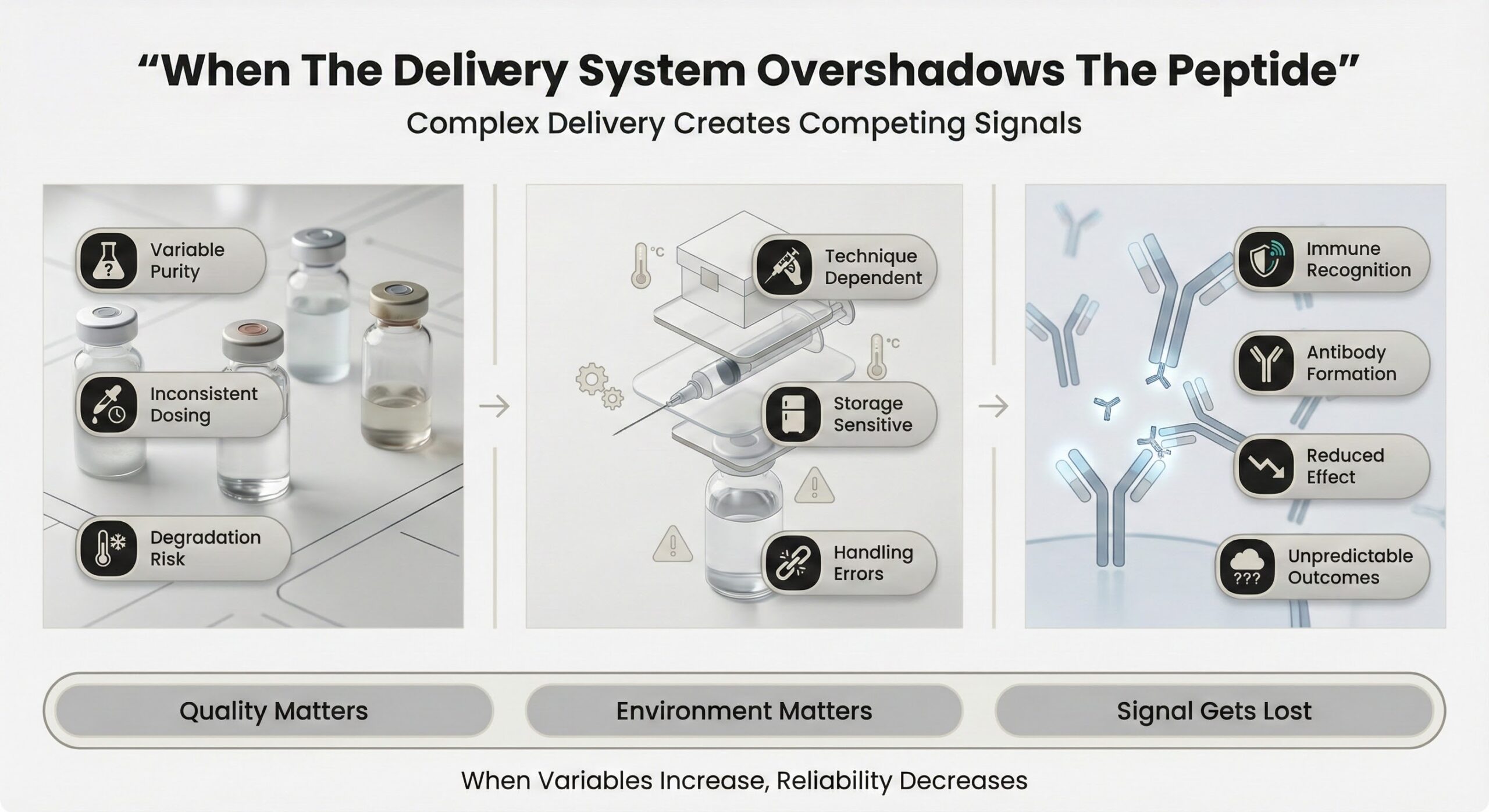
When the delivery system overshadows the peptide
Because many wellness‑oriented injectable peptides are sourced outside tightly controlled pharmaceutical channels, users must think carefully about product quality and handling. If a vial contains impurities, inconsistent dosing, or degraded peptide, even perfect injection technique will not deliver the expected outcomes, and contamination can produce local or systemic immune reactions rather than the intended tissue‑level benefits.[2]
Repeated exposure to synthetic peptides can also provoke the immune system to form antibodies against them, which may gradually reduce or neutralize their effect and, in rare cases, interfere with related natural signaling pathways. In practice, this means the more complex and variable the delivery environment—technique, storage, purity—the more opportunities there are for the body to react to something other than the intended signal, and the less predictable the real‑world benefit becomes.
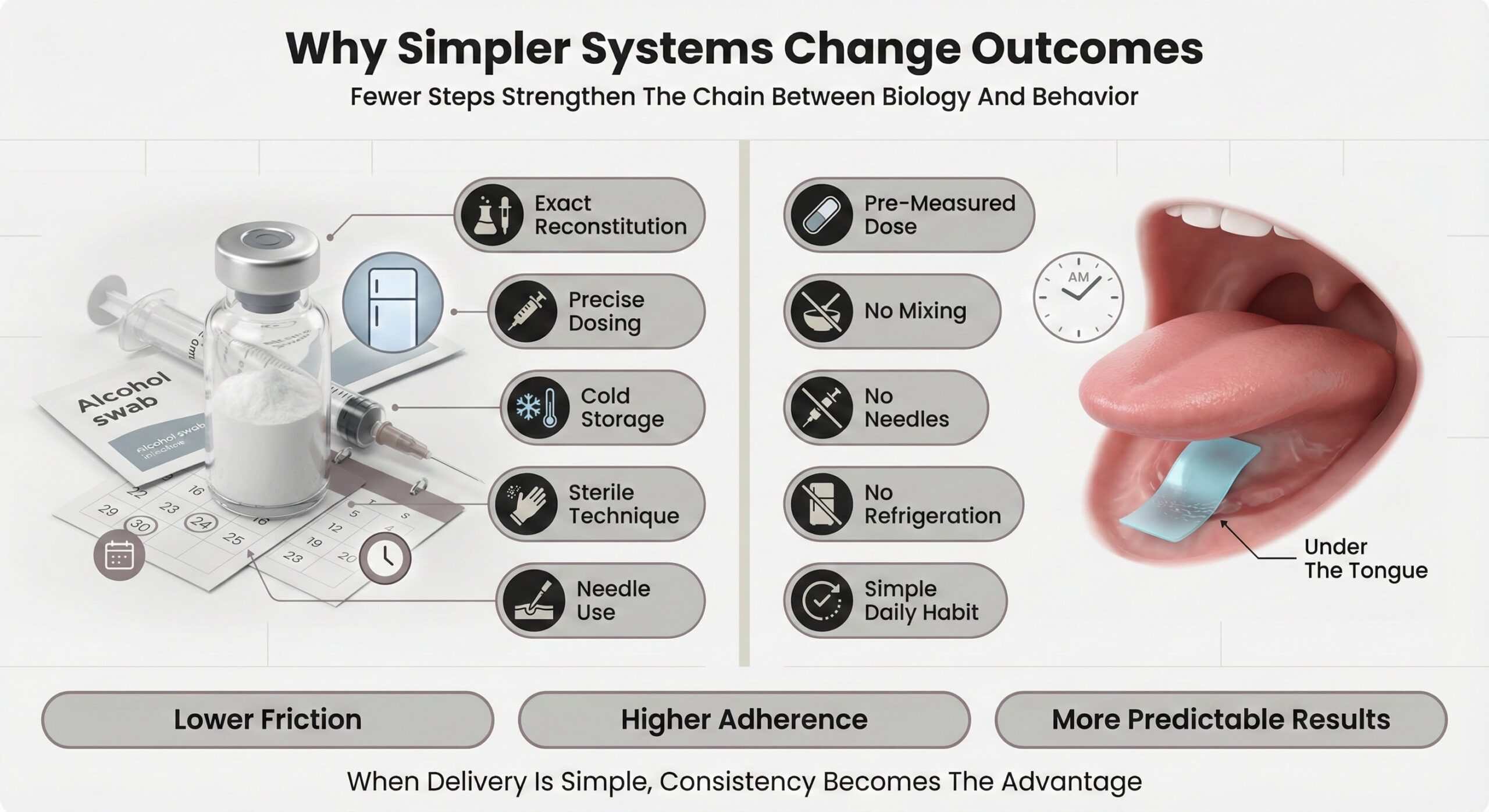
Why simpler systems change outcomes
The core problem is not that injectable peptides “do not work,” but that they demand near‑perfect behavior: exact reconstitution and dosing, reliable refrigeration, strict sterile technique, and ongoing willingness to use needles. Each of those requirements is a potential break in the chain between what a peptide can do biologically and what a person actually experiences day to day.[2]
Dissolving oral strips remove most of these moving parts by delivering pre‑measured doses that simply dissolve in the mouth, with no mixing, needles, or cold storage after manufacturing. Sublingual routes bypass much of the digestive breakdown that limits traditional oral peptides and can reach bioavailability levels several‑fold higher than standard swallowing alone, with reports of sublingual formulations in some contexts approaching or exceeding a third of the exposure seen with conventional oral dosing. When a person only has to place a strip on the tongue at the same time every day, adherence becomes more about a simple habit than a technical procedure—which is exactly the environment where peptides, taken at stable doses over time, can reliably deliver their intended benefits.
References
- Cushman CJ et al. "Local and Systemic Peptide Therapies for Soft Tissue Regeneration: A Narrative Review." Yale J Biol Med. 2024. [View Study]
- [View Study]
- Love AS et al. "Considering Needle Phobia among Adult Patients During Mass COVID-19 Vaccinations." J Prim Care Community Health. 2021. [View Study]
- Alsbrooks K et al. "Prevalence, causes, impacts, and management of needle phobia: An international survey of a general adult population." PLoS One. 2022. [View Study]
Read More

What GMP Certification Means for Supplement Quality
March 10, 2026
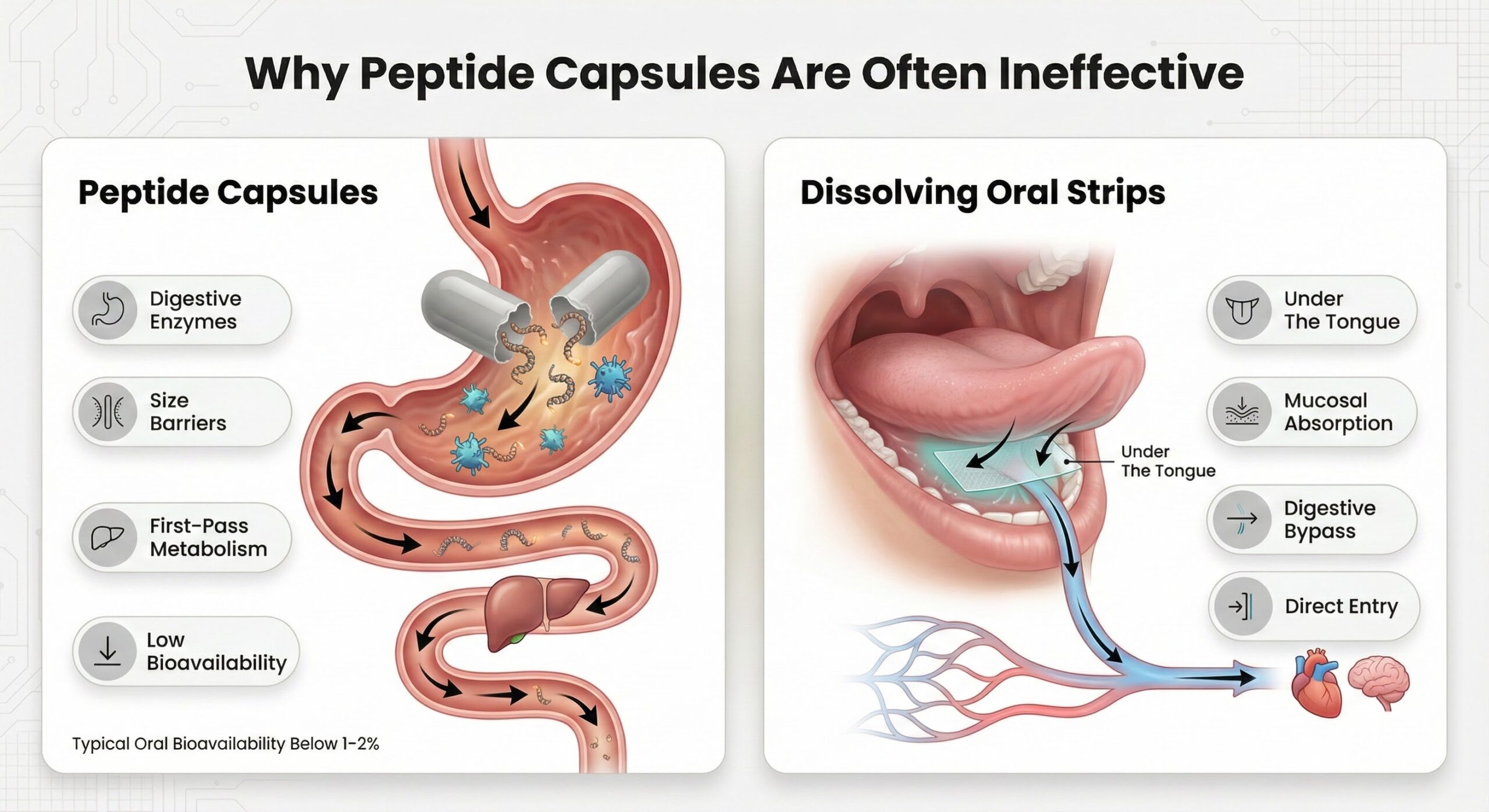
Why Peptide Capsules are Often Ineffective
March 10, 2026
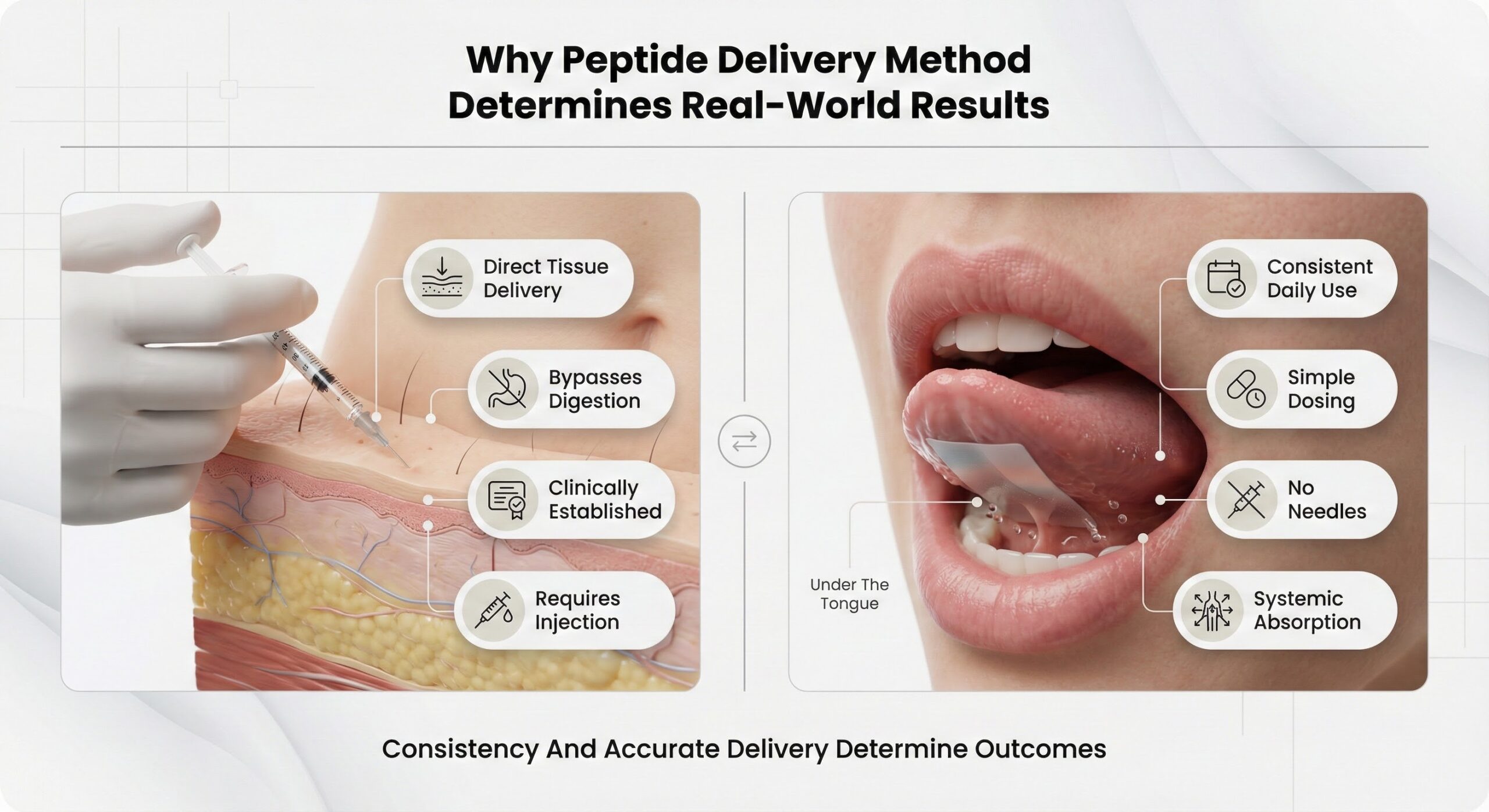
Why Peptide Delivery Method Determines Real-World Results
March 10, 2026





