
Oral Peptide Strips vs Injections: What’s the Difference?
Peptides offer measurable benefits for recovery, tissue repair, metabolic function, and cellular health. But whether you actually experience those benefits depends less on the peptide itself and more on how consistently and accurately it reaches your system. The difference between injectable peptides and dissolving oral strips isn't just about convenience—it's about execution reliability, daily adherence, and whether your delivery method supports or undermines your treatment goals.[1]
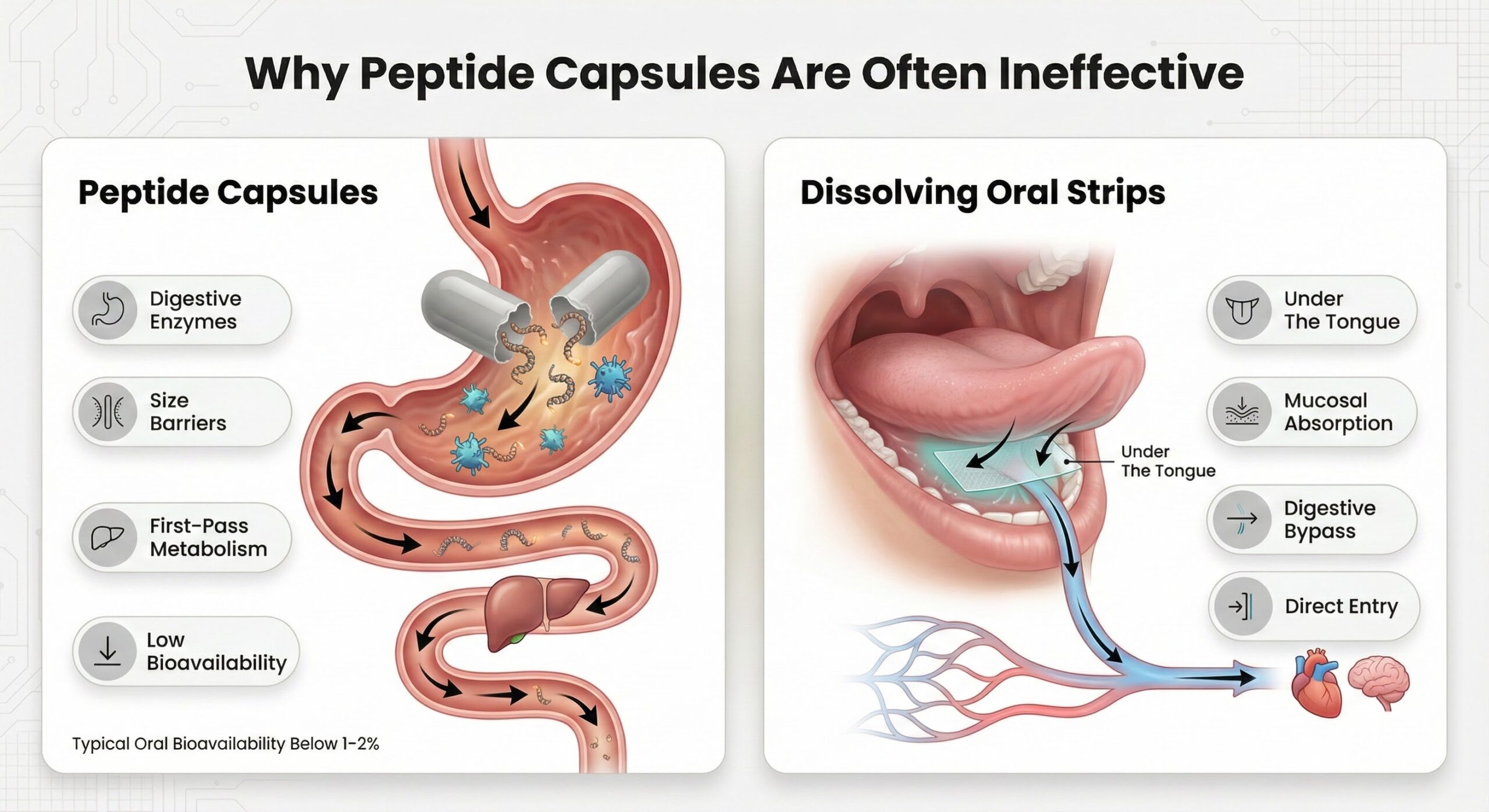
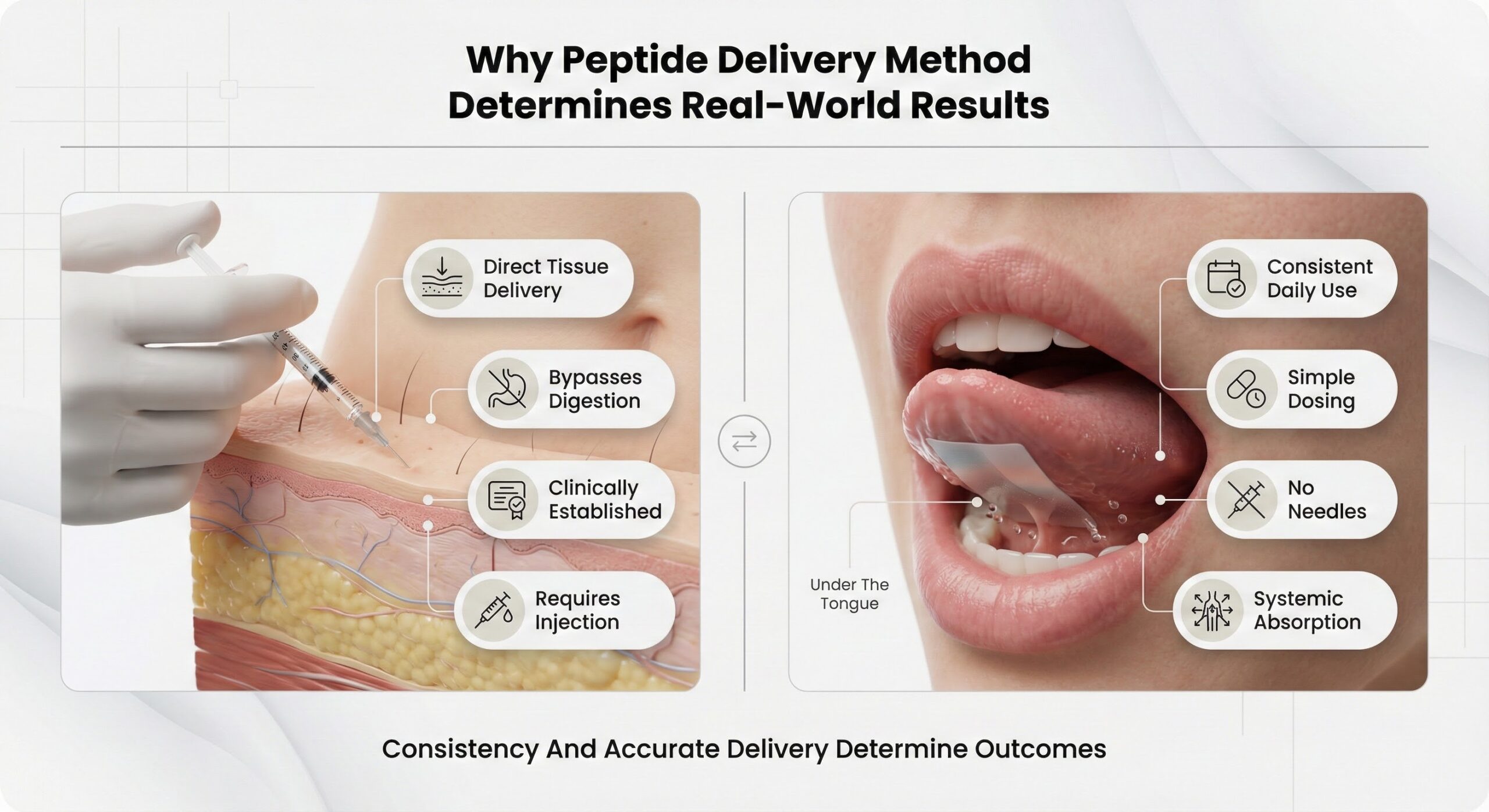
Injectable peptides have been the clinical standard because they bypass digestive barriers entirely, delivering near-complete bioavailability. Oral strips work differently: they dissolve under the tongue, allowing peptides to absorb directly through the oral mucosa into systemic circulation without passing through the stomach or liver. While injections require sterile reconstitution, precise measurement, proper storage, and site rotation, oral strips eliminate these complexity layers—reducing the friction points where dosing errors, inconsistency, and treatment abandonment typically occur. [2]
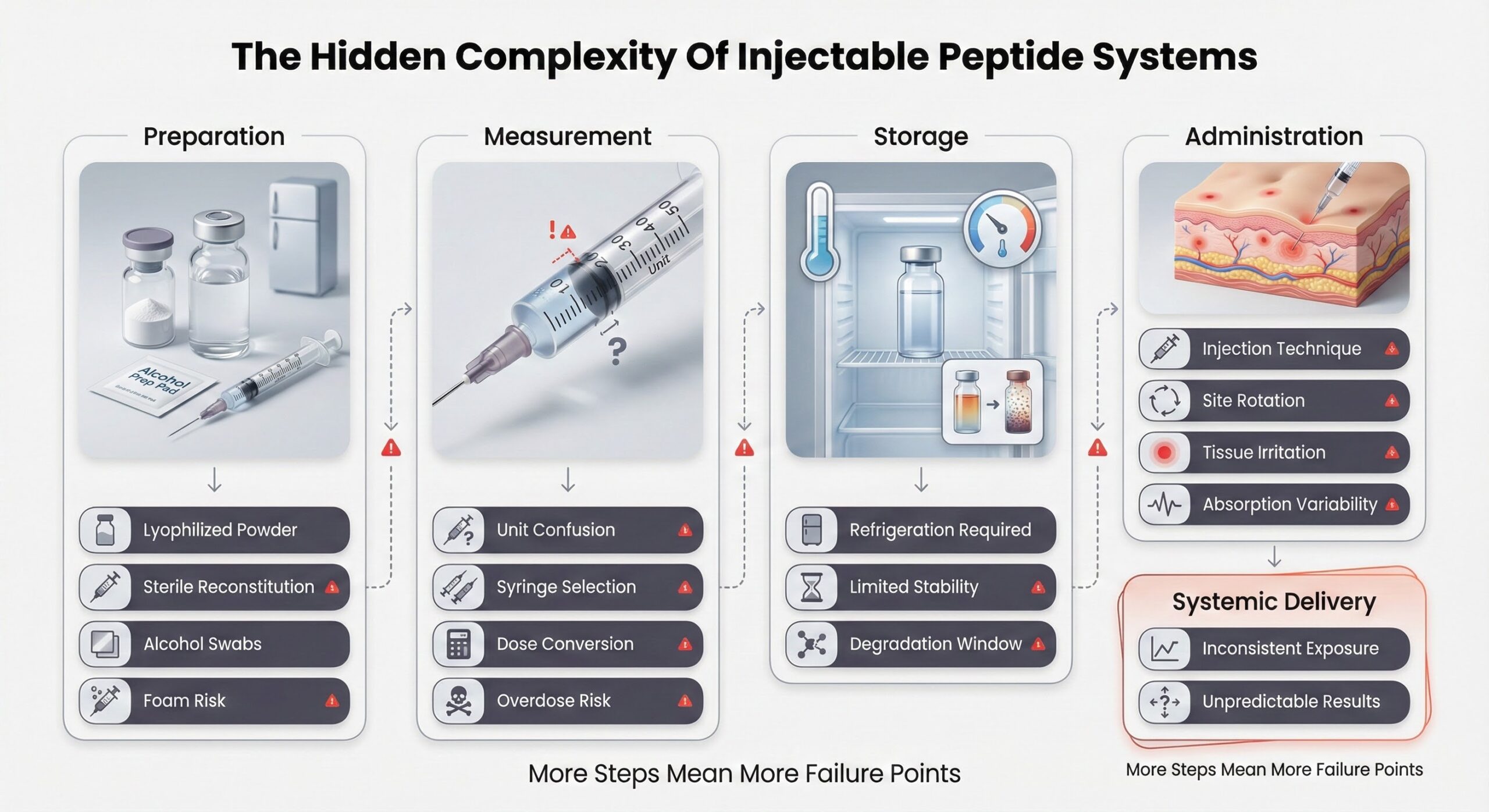
The Hidden Complexity of Injectable Peptide Systems
Injectable peptides arrive as lyophilized powder that must be reconstituted with bacteriostatic water before each use. This process demands sterile technique: cleaning vial tops with alcohol, slowly injecting water down the vial wall to prevent foam, gently swirling without shaking, then drawing the precise dose with an appropriately sized syringe. Once reconstituted, peptides require refrigeration and remain stable for only days to weeks depending on the compound.
Dosing errors with injectable peptides are common and consequential. Reports to the FDA document patients administering 5 to 20 times the intended dose due to confusion about syringe measurements, misunderstanding unit conversions between milligrams and milliliters, or using incorrect syringe types. In one case, a patient was instructed to draw 5 units but mistakenly filled the syringe to 50 units, resulting in a tenfold overdose. Healthcare providers have also miscalculated doses when converting dosing units, prescribing 25 units instead of the intended 0.25 mg (5 units), leading to severe adverse effects including vomiting.
Beyond measurement errors, injections introduce additional failure points. Repeated injections into the same site cause microtrauma, inflammation, and changes in fat tissue density that create lumps or tissue distortion. These changes impair how medication disperses and absorbs, creating unpredictable plasma concentrations that directly affect treatment effectiveness. Proper site rotation across the abdomen, thighs, and upper arms is essential but adds another layer of protocol complexity that patients must remember and execute correctly.
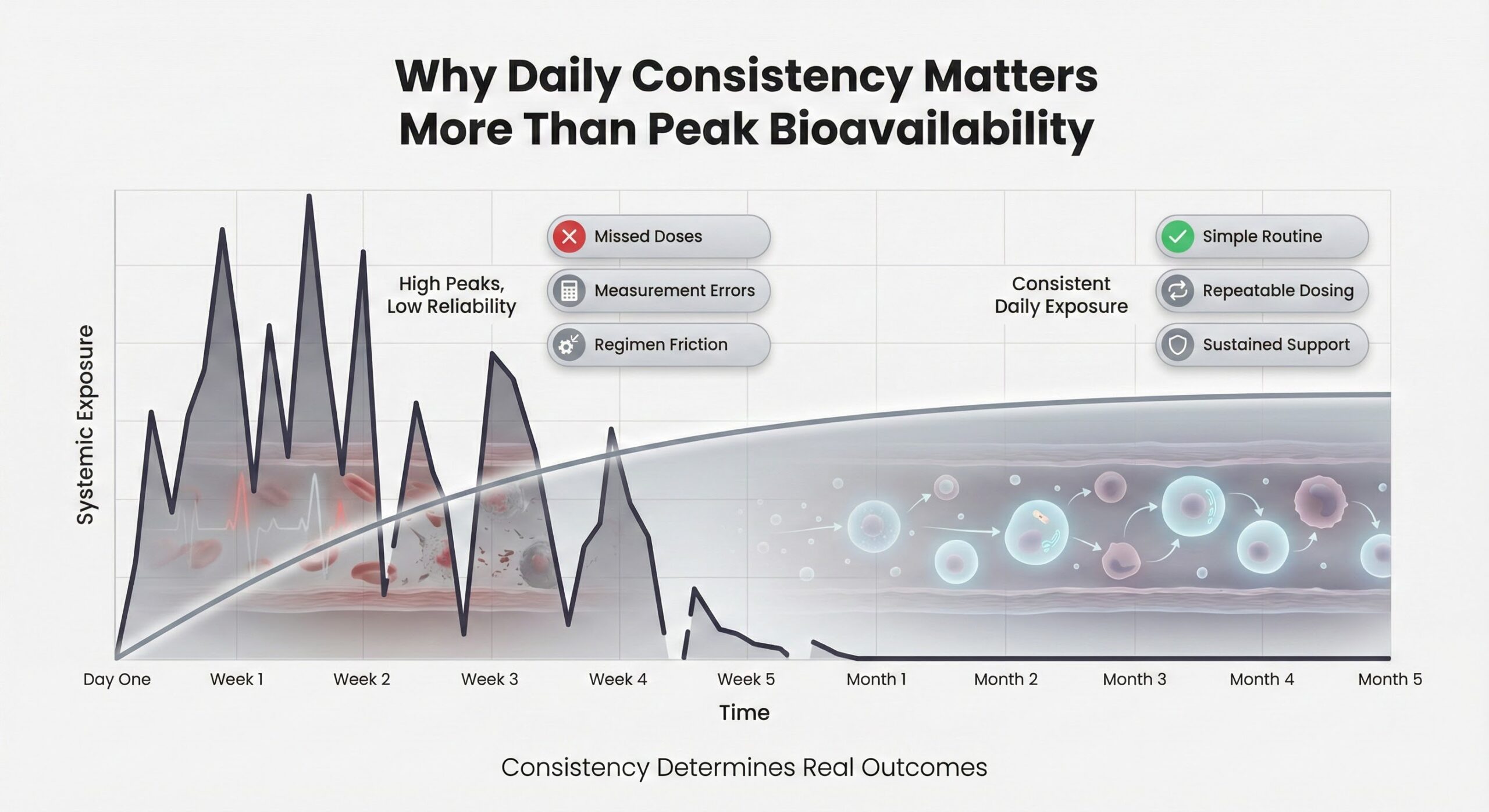
Why Daily Consistency Matters More Than Peak Bioavailability
Peptide therapy produces results through sustained, consistent exposure over weeks to months. The treatment works by restoring balance to physiological systems, addressing underlying imbalances, and promoting cellular repair processes that accumulate over time. A single missed dose or incorrectly measured injection disrupts this continuity.
Research on medication adherence reveals that regimen complexity is one of the strongest predictors of treatment failure. Patients prescribed therapies requiring reconstitution, dose measurement, or multiple daily administrations show significantly lower adherence rates compared to simpler regimens. For injectable therapies specifically, the requirement to draw up insulin doses, split tablets, or manage dosing frequency greater than twice daily creates barriers that reduce real-world treatment success.
The implications are straightforward: if your delivery method introduces opportunities for error, hesitation, or skipped doses, the peptide's theoretical bioavailability becomes irrelevant. Consistent execution determines whether benefits materialize.
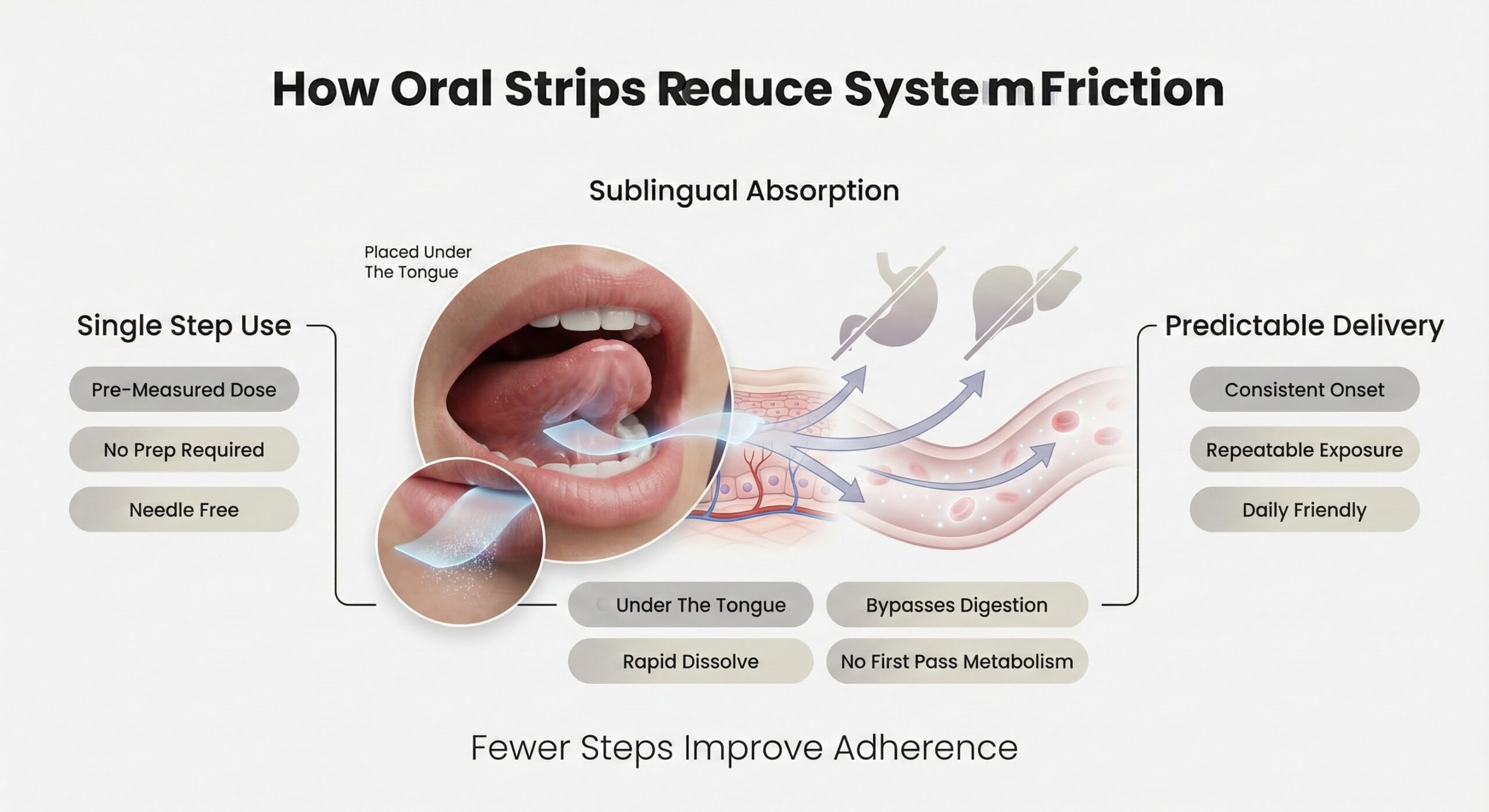
How Oral Strips Reduce System Friction
Oral dissolving strips eliminate the procedural complexity that undermines injectable adherence. Each strip contains a pre-measured, pharmaceutical-grade peptide dose in a thin film that dissolves within seconds when placed under the tongue. There is no reconstitution, no syringe measurement, no refrigeration requirement for unused doses, and no injection site rotation to track.
Sublingual absorption allows peptides to pass directly through the highly vascularized oral mucosa into systemic circulation, bypassing gastric acid and digestive enzymes that would otherwise degrade the compounds. The oral mucosa exhibits substantially lower enzymatic activity than the gastrointestinal tract, and the direct absorption route avoids hepatic first-pass metabolism. Peptides reach detectable plasma levels within 10 to 30 minutes, creating a predictable onset window without the variability introduced by injection-site factors.
From a compliance perspective, needle-free delivery systems show significantly higher patient acceptance and satisfaction compared to conventional injections. Studies evaluating needle-free injection technologies found that patients reported easier administration, less pain, and greater willingness to continue treatment. For populations with needle phobia—which affects approximately 20% of adults—eliminating injection anxiety directly improves adherence rates and long-term treatment sustainability.[3]

The Practical Advantage: Simplified Execution
The difference between strip and injectable systems becomes clearest when examining real-world usage patterns. Injectable peptides require users to maintain sterile technique, accurately measure doses, rotate injection sites, manage refrigerated storage, and dispose of sharps safely. Each step represents a potential failure point.
Oral strips condense this process into a single action: place the strip under the tongue and allow it to dissolve. The pre-measured format eliminates dosing calculation entirely, removing the measurement errors that account for the majority of reported adverse events with compounded injectable peptides. The room-temperature stability of strip formulations removes storage complexity, making consistent daily dosing feasible during travel, at work, or in other non-clinical settings.
Research on medication adherence consistently demonstrates that reducing regimen complexity improves outcomes. Patients using once-weekly therapies show higher adherence rates than those on daily regimens, and fixed-dose combination therapies outperform multi-medication protocols specifically because they reduce the cognitive and procedural burden of treatment. Oral strips apply this principle to peptide delivery: by minimizing the steps between intention and execution, they reduce the friction that leads to missed doses and treatment discontinuation.
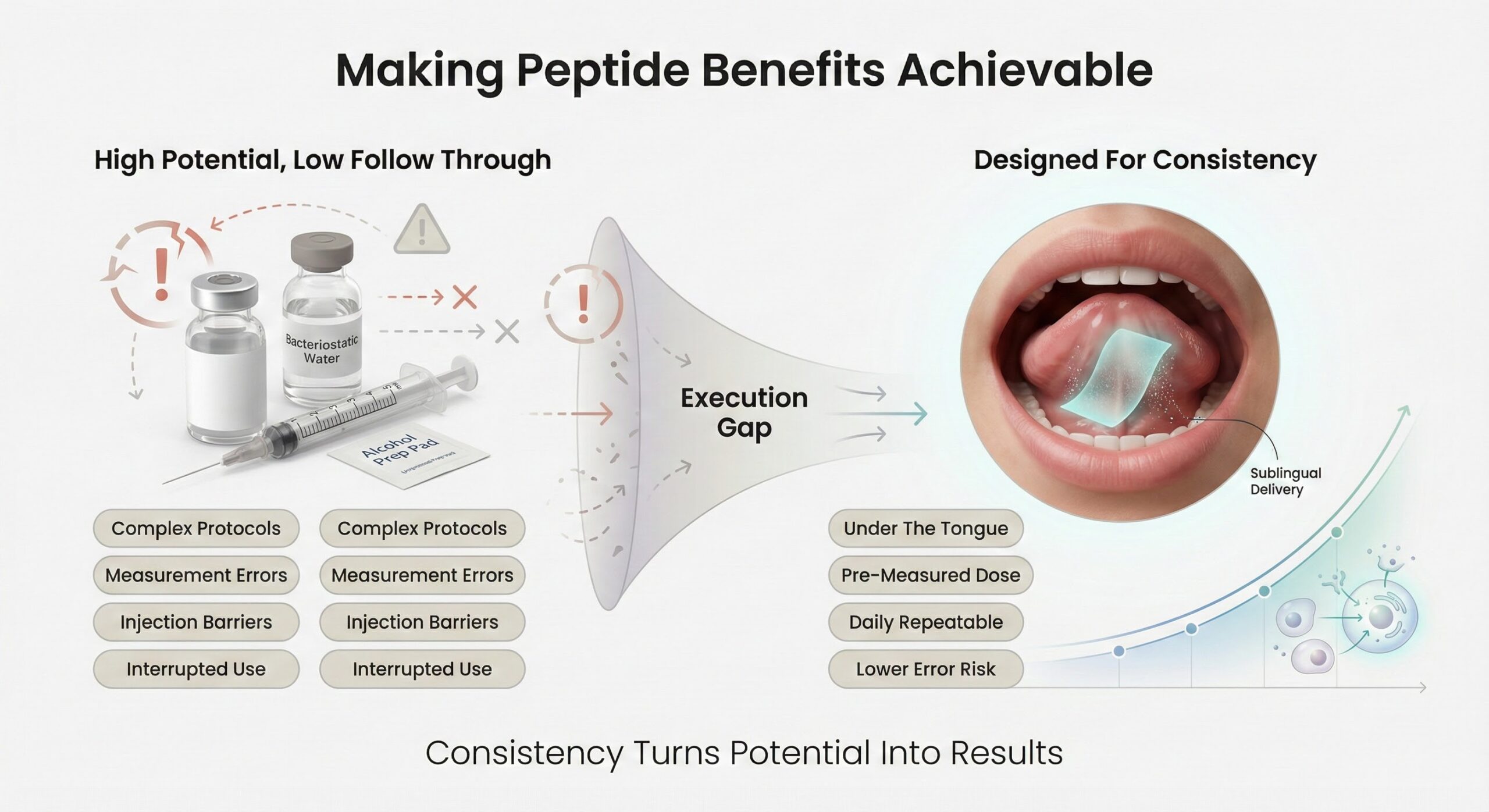
Making Peptide Benefits Achievable
Peptides demonstrate clear therapeutic value for tissue repair, metabolic optimization, and cellular function. But therapeutic potential only translates into experienced benefits when delivery systems support consistent, accurate execution. Injectable peptides offer high bioavailability but introduce procedural complexity, measurement error risk, injection-site complications, and psychological barriers that compromise real-world adherence.[4]
Oral dissolving strips simplify the treatment system by eliminating reconstitution, measurement, refrigeration, and needle handling. The result is a delivery method that reduces user error, supports daily consistency, and removes the execution barriers that prevent people from sustaining peptide therapy long enough to realize its benefits. For peptides that work through accumulated, consistent exposure over time, the delivery system that makes adherence easiest often produces the most reliable outcomes.
References
- Chen G et al. "Oral delivery of protein and peptide drugs: from non-specific formulation approaches to intestinal cell targeting strategies." Theranostics. 2022. [View Study]
- Bruno BJ et al. "Basics and recent advances in peptide and protein drug delivery." Ther Deliv. 2013. [View Study]
- Pathan A et al. "A Pilot Open-Label Randomized Study to Evaluate the Safety, Tolerability, and Acceptability of the IntegriMedical® Needle Free Injection System versus a Conventional Needle-Based System in Healthy Volunteers, Using Normal Saline as a Placebo." Med Devices (Auckl). 2024. [View Study]
- Baral KC et al. "Barriers and Strategies for Oral Peptide and Protein Therapeutics Delivery: Update on Clinical Advances." Pharmaceutics. 2025. [View Study]
Read More

What GMP Certification Means for Supplement Quality
March 10, 2026
Why Peptide Capsules are Often Ineffective
March 10, 2026
Why Peptide Delivery Method Determines Real-World Results
March 10, 2026





